Early morning, August 26, 2009 I was awakened and knew it was time
to go
to the hospital. We made
arrangements to get the girls off to school and
we packed and headed off to St. Vincents Hospital to meet our son,
Noah.
He was originally due September 22 but I knew he was at a decent
weight because I had been to the doctor the previous day. I was a little worried, but not overly
concerned.
Noah arrived in the world the morning of August 26, 2009. He did
not make one
sound whatsoever when he was delivered, which worried me. I continually
asked the doctor if he was ok and she assured me that he was
fine. There
was a small nagging doubt that kept telling me something was
wrong. After awhile, Chris left to check
the girls out of school and I settled in to hold
Noah and rest. The nurse
brought him to me fresh from his bath.
As I
was holding him, I noticed a small blue tinge around his
lips. The
nurse came to check on us and I showed her. She immediately took him
and checked his vitals, reporting that his oxygen was a little
low. She
gave him some o2 and worked with him for awhile. After about 15
minutes, she took him to the nurse’s station so she could keep an
eye on
him. It wasn't long before
she returned (without Noah) and informed me
that he had to go to the NICU because his oxygen kept dropping and
there
was no way for him to be monitored in my room. She asked if the girls
were close to coming and stated that if they were 5 minutes out
they
would wait for them, otherwise he was going on to the NICU. In a panic,
I called Chris to find out that they were in the parking
deck. So the
nurses wheeled Noah in the room in an incubator. I held him while the
girls talked to him, touched him and kissed him. They only let them see
him for 5 minutes then he was wheeled to the NICU. It all happened so
fast, we had no time to process it. The girls kept asking where he went
and why couldn't they see him.
I was extremely upset and it was so hard
to keep composed in front of them.
There were no first family pictures, no pictures of Noah with his
grandparents, nothing but tears and fear. This was the year of the swine flu
and the NICU did not allow anyone except parents to visit. Because of this, nobody except Chris and me got
to see Noah until he was 4 months old.
We were first told that he would be able to go home with me. But the day came and they said, he would stay
another week so I packed up and walked out of the hospital without my
baby. It was the hardest thing I have
ever had to do. We visited daily. It was extremely difficult having a child in
the NICU and 2 children at home. After
the girls left for school, I would drive
to the hospital and stay with Noah until it was time to leave to
meet
the girls at the bus stop.
We would do the regular after school things
of homework and dinner.
When the girls had gone to bed, Chris would go
to the hospital to see Noah.
On the weekends, we would get a sitter and
stay with him a few hours on Saturday and Sunday.
Noah had many different tests (MRIs, Blood Tests, Genetic Tests,
etc). Everything came back normal. He would desat down to the 80s and then
before the nurses could even come check on him, he was back up to the upper
90s. This was constant. He would do this all day and all night and
they couldn't figure out why. He was
eating fairly well. He was fine other than the many desats.
Then, a week after he was born he hit rock bottom. Chris had
gone to see him that evening and he called me when he got to the
hospital. His voice was
shaking and he said they had closed the NICU.
I asked if it was Noah and he said he didn't know because they
weren't
letting anyone back there.
I hung up the phone with him promising to
call me soon. I immediately
knew it was Noah. I just had this
horrible
feeling and a deep blackness overcame me. I began crying hysterically,
trying to keep quiet so as not to frighten the girls. Not too much
later, Chris called me and I have never heard his voice sound so
sad and
scared. He informed me that
Noah had a seizure and they had to intubate
him. We were
terrified. They said his CO2 was too
high and they were
giving him phenobarbital to prevent more seizures (in retrospect
this
was not good because it was depressing his breathing even more but
at
the time we didn't know his diagnosis). The next day, they asked
permission to give him a blood transfusion. They had taken so much
blood from him for tests that he needed more. Seeing him laying there
with a tube down his throat, tape all over his face, iv in his
head,
wires all over and blood on the bed was the most terrifying thing
I had
ever seen. The depression
hit full force and I feared for his life.
This was our life for another week. The doctors would come talk to us
in hushed tones. The nurses
would give us sympathetic looks and pat our
backs. We watched many
babies come and go from the NICU but there we
sat with no end in site. I
began to dread going to the hospital but I
felt so guilty when I wasn't there. It was killing me to see him like
that. He was never awake
and we did not get to hold him. They
stopped
feeding him by mouth and gave him an IV. The lowest day was when the
doctor told us they could not care for him anymore. She informed us
that he was being transferred to our local children's hospital,
which in
retrospect was the best thing that could have happened. With deep pity
in her eyes, she informed us that they suspected that Noah had
Ondine's
Curse or Congenital Central Hypoventilation Syndrome, a very rare
disease. She said that he would be on a
ventilator the rest of his life and would most
likely have to be institutionalized. She said that she had only seen
this extremely rare disease in a child one other time. She handed us a
short 5 paragraph medical paper and told us she would let us
"process the information" and then she walked off. We were devastated. How is a parent suppose to process that
information? They gave us no hope, no
information and it seemed as if they had just washed their hands of him.
Shortly thereafter, Noah was transported by ambulance to
children's hospital. I did not get to go
because I was at the doctor with Hannah, who had the flu. Chris made sure he got settled in and took
some pictures for me. Unfortunately, I got
the flu also and could not visit Noah for 2 weeks. It was truly the worst nightmare.
Once I finally got to visit, the whole atmosphere was different. The nurses were encouraging. Noah was awake and the nurse asked if we
wanted to hold him. In shock, we asked
if we really could and were told that they encouraged it. I finally got to hold him after 2 weeks. The pulmonologist did a sleep study, which
Noah failed miserably.
I remember the day we finally got a diagnosis. We were visiting Noah together (Chris was on
his lunch break) and all of the doctors and nurses gathered around Noah's
bed. I immediately became nervous. The pulmonologist informed us that the test
had came back positive for Congenital Central Hypoventilation Syndrome
(CCHS). I immediately broke down. The doctor kept talking but for a minute
there all I heard was a roaring in my ears.
The fear was overwhelming. I had visions
of having to send him out of state to some institution and never being able to
see or care for him myself. I slowly
began listening to the doctor. He told
us that the diagnosis was scary but that Noah would be up in no time running
around like every other child. He told
us that he would be able to go to school, play ball and do everything else (except
maybe scuba dive). We were told that we
would have to have extensive training before bringing him home and it was still
going to be awhile before he was released from the hospital, months not
days. I was horrified and elated at the same time. We went from being told that he
would live in an institution to being told that he would not only
be going home but that he would live life like any other child. It was an extraordinary amount of information
to process. We went home and got on the
computer, which was a mistake. There
wasn't a lot of information out there and we really felt so alone and
scared.
That evening, we got a call telling us that they wanted to do
trach surgery the next day. We consented
and went to the hospital after getting the girls off to school. The surgery
did not last long and we were able to see him soon after. That first glimpse of him was amazing. For the first time since he had been born, we
saw his little face. It was a little red
from the tape, but he was sleeping so peacefully. The trach looked scary but he looked so
much more comfortable. The
thing that scared us was that his breath
rate on the vent was up to 55 bpm and he was not taking any
breaths on
his own. The ventilator was
taking every breath for him. They
informed
us this was because of the sedation.
The next day, he was awake and alert. His breath rate was down. After about a week, they told us that he
would be moved to a floor as soon as they had a bed for him. We were so excited. This was one more step closer to coming home
and the girls could finally come visit him.
The day finally arrived and he went to the pulmonary floor. What an amazing day. The girls got to hold and snuggle with him
and we finally got some pictures of them together. He
was 2 1/2 months old. We
still could not stay there with him because the room he was in had no bed for
us but at least we could let the girls visit whenever we wanted and stay as
long as we wanted.
The nurses slowly began showing us how to suction and we began
asking a lot of questions. The home
ventilator team met with us and explained exactly what would happen. We decided
to allow him to have a g-tube so that we would get to take him home
quicker. He was eating, but not enough
to sustain him. They felt that this was
because he had been IV fed for so long.
After the g-tube and trach site had healed some, we would begin
our training and train for 3 days a week for a few hours. Our training included doing
everything 3 times each (bathing, cleaning the trach, changing the
trach, suctioning, changing the circuits, doing a bolus feed,
etc). We
decided that I would train while Chris worked, since he was our
only
source of income. My mother
and mother in law agreed to be trained as
well.
We began our training on my birthday, which was the best present
ever. For the next month,
we learned as much as we could. We had
an
excellent home vent nurse who made sure were were thoroughly
trained.
We learned in one month what it took professionals years to
learn. We
took lots of notes and knew that we were not eligible for nursing
care
at home so we paid close attention. We learned quickly and they told
us they would try their best to have us home before
Christmas.
December 15, 2009 was Noah's homecoming. It was a day we never thought we would see. The homecoming was a little crazy because
Hannah had a stomach
virus and the DME had to meet us ASAP because Beth had her first
band
concert. My mother in law
stayed with Noah while we went to the
concert. The first night
home, I didn't sleep at all. Our dining
room
looked like a mini ICU. We
had him hooked to the vent, pulse ox, apnea
monitor, and feeding pump.
He looked like a little science experiment
laying there but we didn't care.
He was finally home.
Slowly, we began to get in to a routine. I was able to wean him off the vent. I realized that I could do this. Then, he got sick. Never had he had
oxygen in the hospital but now he needed oxygen. I was so extremely
stressed for the week he was sick.
He was ventilated 24/7 and I was
constantly suctioning and dealing with alarms. Christmas day, he slept
a lot. We really didn't
care because we were all together.
Eventually,
he got better and our routine returned to normal.
3 months after coming home, we took our first trip to the
beach. It was the most amazing trip we
have ever had. He loved it and we were
elated to
realize that we could do this and live a relatively normal
life. The
darkness was over.
Noah is now a happy, healthy 3 year old. He is off the vent during the
day and we trach his cap.
His speech has improved greatly after 3 years of speech therapy and he
has proven to be so smart with a great sense of humor. He is our miracle and our blessing. We have learned so much from him. I never tire of hearing him run around the
house aggravating his sisters and being a real boy. I never thought we would
get this far. We do not know what the
future holds. Hopefully we will be able
to have him decannulated and just use a bipap.
We may even do the diaphragm pacer surgery. Attending school is our next big hurdle.
Life is never boring with our little miracle man. We are always doing research on CCHS, constantly
having struggles with the equipment company, insurance, and doctors. Slowly, we have learned how to live with a
special needs child. It has been rough
at times but worth every minute.
 |
| Before the CCHS diagnosis |
 |
| Our first pictures together |
 |
| After trach surgery |
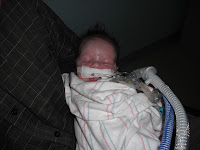 |
| Before trach surgery |
 |
| Noah age 3 |
 |
| At the beach |
 |
| At the park |
No comments:
Post a Comment